Next-Level Medical Credentialing, Powered by AI
ClinicConnection™ is a cloud-based risk management and work management platform designed for next-level medical credentialing programs. Proactively manage credentialing risk, automate tedious processes, and quantify the revenue impact of every credentialing delay.

I love supporting a clinic owners’ pursuit of achievement. I found that creating and maintaining a successful credentialing program was one of the most difficult tasks a clinic owner would face. And so, I created Therapy Credentialing Services to help clinic owners focus on their strengths.
Now, healthcare practices can retain their in-house credentialing program and opt to use ClinicConnection™ as a solution.
When I first started my clinic I was forced to use spreadsheets to manage data and couldn’t manage credentialing risks effectively or efficiently. My drive, motivation, and ambition prompted me to build something better. Now I bring it to you.
— Megan Hart, CEO
Revenue Readiness Dashboard
See the exact dollar impact of credentialing delays — in real time.
- Hero Metric Dashboard — Six financial KPIs at a glance: weekly blocked revenue, cumulative missed revenue, fully credentialed count, projected impact, employee burden costs, and ramp-adjusted calculations. Know exactly what credentialing delays are costing you.
- Payer Bottleneck Analysis — Instantly identify which insurance payers are causing the most revenue delays across your entire organization. See total blocked revenue per payer and average days pending so you can prioritize follow-ups.
- What-If Simulation Engine — Model hiring scenarios before committing. Add hypothetical providers, adjust payer approval timelines, and override visit volumes to forecast financial impact before you make a single hire.
- Snapshot & Trend Tracking — Capture point-in-time financial snapshots and track 90-day trends. Prove to leadership that your credentialing process improvements are moving the revenue needle with hard data.
- Cross-Group Portfolio View — Executive-level summary across all clinic groups. Compare group-to-group credentialing velocity, benchmark by specialty or payer, and spot the outlier groups that need attention.
Generate PDF Credentialing Apps
Generate filled-in insurance credentialing PDFs for hundreds of providers in seconds.
- Batch PDF Generation — Queue and generate credentialing applications for one or hundreds of providers simultaneously. Templates auto-populate from your provider and group data — no more manual form filling or data transposition errors.
- AI-Assisted Editing — Use natural language commands to make corrections: “Change the NPI to 1234567890” or “Update the effective date to March 1.” See before-and-after values for every change before you accept.
- Template Management System — Upload payer-specific PDF templates (Humana, Optum, ASH, ATA, and more) with precision field mapping. Support template variants per group and payer combination for maximum flexibility.
- Review Queue with Inline Preview — Split-screen review: PDF preview on the left, metadata and AI editing on the right. Accept, reject, or edit applications before submission with full audit trail.
- Automatic DMS Integration — Accepted applications automatically create document records linked to both the provider and group. No manual filing — everything flows into your document management system instantly.
Draft
Edit
Reject
Smart Document Management
AI-powered document hub that classifies, extracts, and organizes your credentialing files.
- AI Quick Upload Wizard — Drag-and-drop upload with automatic document classification. AI pre-fills title, description, document type, and expiration dates. Multi-page PDFs are automatically split into individual documents with intelligent boundary detection.
- Provider Matching from Content — AI reads uploaded documents and matches them to providers by extracting NPI, CAQH numbers, and names from the document text — complete with confidence scoring so you know how reliable the match is.
- OCR & Text Extraction — Azure Document Intelligence extracts searchable text from PDFs and scanned images. Every document becomes searchable across your entire organization — find any document in seconds.
- Expiration Date Tracking — Documents with expiration dates are automatically flagged. Combined with business rules, expired licenses and insurance policies trigger proactive alerts before they impact your credentialing program.
- Rejected Document Review Queue — Split-screen review interface for flagged documents. Correct metadata and navigate to the next item seamlessly. Batch your way through document review in minutes, not hours.
FL State License – Johnson
State License
Sarah Johnson, LCSW (NPI match)
01/15/2027
Secure File Requests
Collect provider documents securely — no login required for your providers.
- Multi-Step Onboarding Wizards — 9-step provider onboarding and 12-step group onboarding wizards with progress saving. Recipients can complete forms over multiple sessions without losing their work.
- Automatic AI Classification — Uploaded files are automatically classified by document type (license, insurance, certification, background check) during submission — no manual sorting needed.
- Email & In-App Notifications — Admins receive instant alerts when files are uploaded. Recipients get branded email invitations with their secure link and confirmation notices when submissions are processed.
- Review & Convert Workflow — Review submissions, accept to automatically create provider or group records, or reject with feedback. Selectively attach documents to existing entities for maximum flexibility.
Secure Document Submission
Sunshine Therapy Group — Provider Onboarding
Continue
NPPES & Real-Time Data Integration
Verify provider data against the national registry in real time. Stop scouring and transposing data.
- Live NPPES Registry Search — Search the CMS NPPES database directly from ClinicConnection by name, NPI, or postal code. Auto-populate provider and group forms with verified data — get the data right from its source.
- Bulk Verification & Discrepancy Detection — Verify all providers and groups on a schedule. Flag changes in NPI status, taxonomy, or address. Catch problems before they derail a credentialing application.
- Duplicate NPI Detection — Automatically check for duplicate NPIs before importing a provider. Prevent duplicate credentialing records and data conflicts across your organization.
- Smart Sub-Entity Extraction — One NPPES import automatically creates DOH license records, Medicaid profiles, and GroupNPI records from taxonomy and identifier data. One click, complete credential trail.
- Multi-Source Data Aggregation — Capture provider datasets from DOH, NPPES, State Medicaid, and Medicare. View it all on one screen. Get alerted to changes like Medicare Revalidation Due Date updates or Medicaid Next Reval Date shifts.
Active
Active
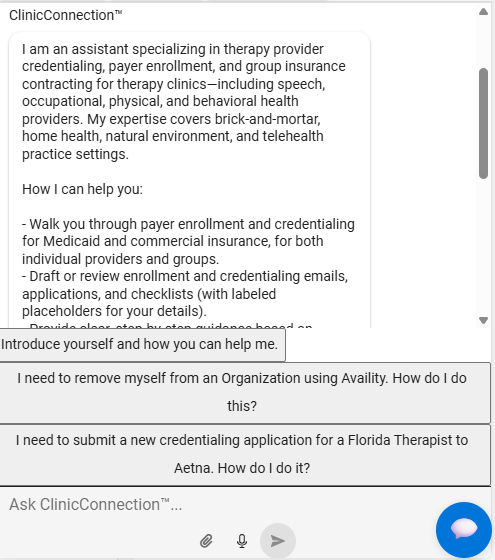
AI Credentialing Agent
Give every team member their own expert credentialing AI advisor.
- Domain-Expert Knowledge — AI advisor with deep knowledge of payer-specific credentialing, enrollment, and contracting. Ask “How do I enroll with UnitedHealthcare?” or “What’s required for Medicaid for ABA groups?” and get actionable, step-by-step answers.
- Document-Aware Analysis — Attach PDFs, images, or documents to your questions. AI extracts and analyzes content: “What’s missing from this application?” or “Extract the key dates from this license.” No more squinting at fine print.
- Persistent Conversations — Multi-turn conversations with full history. Pin important messages for quick reference. Resume discussions across sessions so your team never loses context.
- Template & Draft Generation — AI generates credentialing letters, deficiency notices, enrollment follow-ups, and payer outreach emails with data placeholders. Stop starting from scratch on every communication.
- Step-by-Step Workflow Guidance — AI provides payer-specific enrollment steps with estimated processing timelines and escalation contacts. Every team member gets expert-level guidance, regardless of experience.
Business Rules & Compliance Engine
Automated compliance checks catch issues before they cost you.
- Configurable Rule Sets — Define validation rules without code changes. Rules cover universal prerequisites, payer-specific requirements, revenue readiness, and pre-credentialing checks. Add or modify rules as payer requirements evolve.
- Four-Tier Severity System — Blocking Errors, Overridable Errors, Warnings, and Tasks. Color-coded dashboard badges help your team prioritize what to fix first — and what can wait.
- Smart Context-Aware Rules — Rules evaluate multiple conditions simultaneously. Example: “If Medicaid product AND specialty is RBT AND BACB certification not uploaded, then Error.” Each rule cites its source documentation for easy reference.
- Pre-Credentialing Automation — Validation automatically triggers NPPES re-verification if data is more than 30 days stale. Rules enforce payer prerequisites before applications can be submitted — preventing wasted effort on incomplete submissions.
- Resolution Tracking & Audit Trail — Track which violations were resolved, overridden, or still pending. Maintain a complete history for compliance audits and regulatory reviews.
2 Warnings
8 Passed
1 Task
State License Expired — FL license expired on 02/28/2026. Provider cannot be credentialed with any payer until renewed.
Source: Universal Prerequisites §1.1
Background Screening Missing — No BGS Level 2 document on file. Required for Medicaid enrollment.
Source: Universal Prerequisites §4.1
BACB Certification Expired — BACB cert expired 02/28/2026. Required for ABA credentialing.
Source: Universal Prerequisites §8.1
CAQH Re-Attestation Due — Last attestation was 95 days ago. Re-attest within 120 days to maintain active status.
Liability Insurance Expiring Soon — PLI expires in 28 days (05/05/2026). Begin renewal process now.
Upload Updated Resume — CV on file is more than 12 months old. Consider requesting an updated version.
NPI Verified — NPI 1234567890 confirmed active via NPPES (verified 2 days ago).
Credentialing Gantt Chart & Timeline
Visualize your entire credentialing pipeline at a glance.
- Interactive Timeline Visualization — Gantt chart displays provider credentialing timelines grouped by payer, specialty, or anticipated approval month. See your entire pipeline from hire date to credentialing completion.
- Color-Coded Status Bars — Green (credentialed), blue (submitted), orange (in progress), red (denied), gray (not started). Instantly spot which providers and payers are bottlenecking your revenue.
- Hierarchical Drill-Down — Provider → Payer → Phase → Milestone. Click through layers to understand exactly where delays are occurring and why.
- Multiple Time Views — Switch between day, week, and month perspectives. Group by specialty, payer, or anticipated approval month to answer different strategic questions at a glance.
Credentialed
Submitted
In Progress
Denied
Not Started
Provider & Group Management
All your credentialing data — providers, groups, payers, panels — in one unified hub.
- Unified Profile Hub — All provider and group information in one place: contacts, credentials, NPI, licenses, Medicaid IDs, insurance, and payer panels. No more bouncing between spreadsheets and portals.
- Inline Sub-Object Management — Edit DOH licenses, Medicaid profiles, liability insurance, certifications, and notes directly on the profile page without page reloads. Fast, efficient data entry for busy credentialing teams.
- Panel & Payer Tracking — Track credentialing status per payer: Credentialed, Non-Cred, Needs App, Processing, Terminated. Plan enrollment strategies with historical processing data so you know what to expect.
- Multi-Location & Multi-Discipline Support — Manage multiple clinic locations, specialties (ABA, Speech, OT, PT), and provider types. Track facility certifications, ownership structures, and group-level compliance across your entire organization.
Aetna
Cigna
Medicaid
United
BCBS (denied)
Partner API & Integrations
Connect your EHR, MSO, or staffing platform directly to ClinicConnection.
- RESTful API with Secure API Keys — Partners authenticate via Bearer token with full audit logging of every API call for accountability.
- Multi-Tenant Isolation — Each partner sees only their own groups, providers, and payer data. Complete data segregation ensures no cross-partner data leakage.
- Programmatic CRUD Operations — Create groups, manage providers, sync credentialing status, and query revenue readiness data programmatically. Build custom dashboards or sync with your existing systems.
GET /api/v1/providers/1234567890/status
// Headers
Authorization: Bearer sk_live_a1b2c3…
Content-Type: application/json
{
“npi”: “1234567890”,
“name”: “Sarah Johnson”,
“credentialedPayers”: 4,
“pendingPayers”: 2,
“blockedWeekly”: 2480.00,
“readinessScore”: 0.69
}
Payer Directory & Contact Management
Never lose a credentialing contact again.
- Comprehensive Payer Profiles — Track payer legal names, NPIs, addresses, websites, and processing timelines. Build an institutional knowledge base that stays even when team members leave.
- Multi-Level Contact Directory — Store primary enrollment contacts, escalation contacts, and department-specific numbers. Even track IVR directory tree sequences so your team navigates automated phone menus faster.
- Payer-Specific Requirements — Link unique document requirements and business rules per payer. Know exactly what Humana needs vs. Medicaid vs. CareSource — before you start the application.
- Agreement & Contract Tracking — Store provider agreements and master group contracts with signature dates, effective dates, and renewal reminders. Never miss a contract renewal deadline.
Insurance Payer
Government
Insurance Payer
Activity Logging & Compliance Audit Trail
Complete accountability for every action in your credentialing program.
- Every Change Tracked — Create, update, and delete operations are logged with before-and-after values, timestamps, and user attribution. Know who changed what and when — always.
- Dual Notification System — Real-time in-app notifications plus email alerts for critical events: file uploads, request completions, expirations, and status changes. Stay on top of your credentialing program without constantly checking.
- DOH Monitoring — Monitor and detect your providers’ presence (or absence) in Department of Health Disciplinary and Administrative Actions search results. Catch issues before they become crises.
- Export-Ready Audit Logs — Export activity logs and audit trails for compliance reviews and regulatory reporting. Your credentialing timeline is always documented and defensible.
Three Steps to a Better Credentialing Program
Centralize
Import and organize your credentialing data from multiple sources — NPPES, DOH, Medicaid, Medicare, CAQH, and your own records — into one unified platform.
Automate
Let AI and business rules handle document classification, compliance validation, PDF generation, and data verification. Your team focuses on decisions, not data entry.
Optimize
Track revenue impact, identify payer bottlenecks, model hiring scenarios, and prove ROI to leadership with hard data — not guesswork.
Designed for Clinics That Mean Business
ClinicConnection™ is purpose-built for the unique challenges of healthcare credentialing at scale.
Multi-Location Clinics
Large multi-disciplinary, multi-location therapy practices that need centralized credentialing oversight.
ABA & Behavioral Health
ABA, Speech Therapy, OT, and PT practices with complex payer enrollment and BACB certification tracking.
Clinic Owners & Managers
Owners and credentialing teams who need visibility into risk, revenue impact, and compliance status.
MSOs & Staffing Agencies
Management services organizations and staffing agencies that manage credentialing across multiple providers via our Partner API.
Ready to Transform Your Credentialing Program?
For more information, to schedule a demo, or ask about pricing — we’d love to hear from you.
